CONVERSATION INTELLIGENCE FOR HEALTH INSURANCE
Measurable performance gains, driven by real conversations
Members reach out to you in times of stress—when benefits are unclear, authorizations are denied, or certainty feels out of reach. Turn moments of member frustration into powerful insights and solve operational problems at the source.

Turn moments of friction into member satisfaction
Purpose-built for health insurance
Deploy faster within weeks—not months—using models purpose-built for enterprise payers. Improve Star Ratings, strengthen CAHPS performance, and stay audit-ready with no complex configuration or keyword libraries required.
Foresight you can act on
Detect early signals of churn, dissatisfaction, and compliance risk across 100% of interactions, so you can prepare for enrollment cycles and regulatory shifts before they impact performance.
Reality-driven transformation
Move beyond assumptions and averages. Use real member conversations to improve quality, strengthen retention, and earn long-term member trust.
Business Insights
Business-critical intelligence
System-level insight reveals what’s driving enrollment, retention, and dissatisfaction across your member experience.
Quality & Coaching
Scale quality. Grow confidence.
Healthcare-trained AI scales QA and coaching across every interaction to ensure agents deliver consistent, compliant, high-impact member support.
Safety & Compliance
Detect risk early. Act with confidence.
Monitor 100% of member interactions to surface compliance risk, privacy issues, and safety signals—giving your team confidence in audits, oversight, and regulatory readiness.
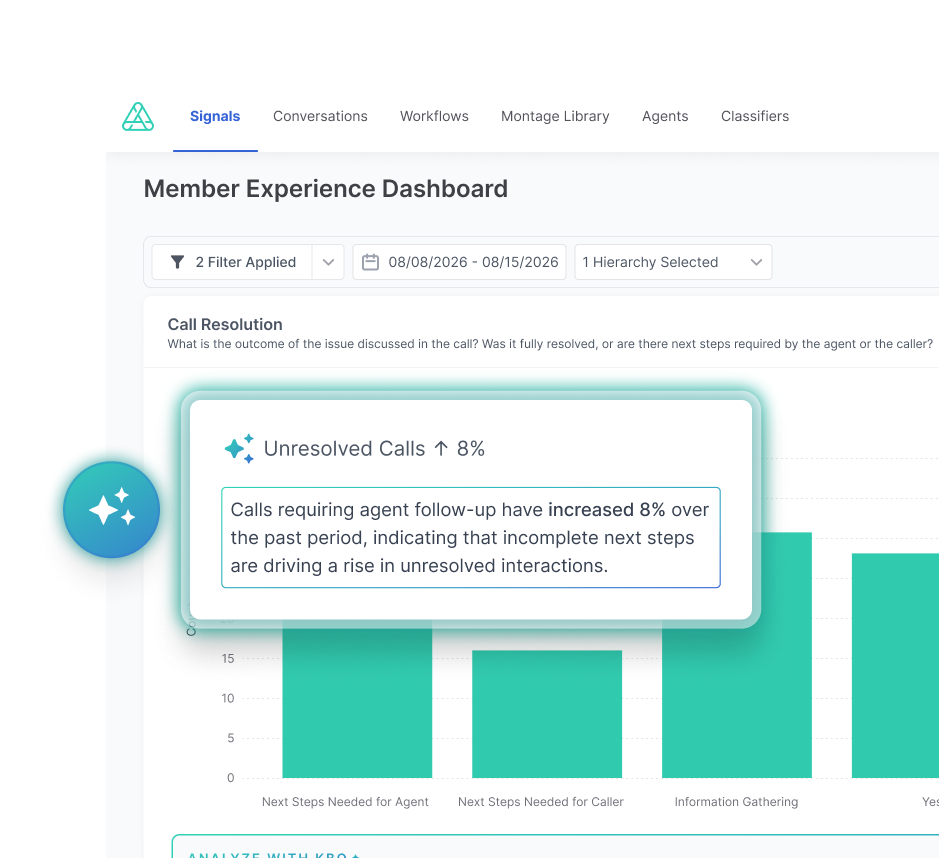
POSITIVE MEMBER IMPACT
Understand leading drivers of dissatisfaction and churn to retain and grow.
CONVERSATION INTELLIGENCE FOR HEALTH INSURANCE
Trusted insights for Medicare providers

Quantify and contextualize how members and providers navigate your process to best anticipate a positive Medicare star rating.

Identify and address leading drivers of member attrition year over year.

Gain valuable context on why members stop or change coverage plans to address brand detractors ahead of open enrollment.
“Saved our company significant amount of time and money”
“It’s helped us identify trends in member interactions more efficiently and has streamlined our QA process in a big way.”
Anonymous
Health Insurance Member
“Every possible angle”
“Overnight, we went from a higher-level understanding of what was happening in our call centers to being able to look at our calls from every possible angle.”
Anonymous
Health Insurance Member
“The source of truth”
“We have gained better visibility into the member experience and been able to drive better outcomes based on the insights we are gathering from interactions.”
Anonymous
Health Insurance Member
Frequently asked questions
Conversation intelligence uses AI to analyze member conversations across voice, chat, and digital channels to uncover patterns, friction points, and risks buried in unstructured data. For health insurance organizations, it turns everyday interactions into actionable insights that improve experience, enhance quality, and ensure compliance.
Conversation intelligence reveals where members get confused, frustrated, or stuck, so healthcare payers can fix issues at the root cause. By acting on real member feedback, organizations reduce repeat calls, improve member satisfaction, and deliver clearer, more supportive experiences.
Purpose-built, healthcare-trained AI listens at scale, identifying intent, nuance, and safety signals that generic tools miss. It connects millions of interactions into clear patterns that guide smarter decisions and confident action.
Chatbots respond to individual interactions. Conversation intelligence analyzes all interactions across every channel and touchpoint to uncover systemic issues, risks, and opportunities, providing enterprise-level clarity, not momentary responses.
In payer call centers, conversation intelligence helps scale quality assurance, identify coaching opportunities, and improve first-call resolution. It also surfaces systemic issues—like benefit confusion or process breakdowns—that drive unnecessary volume and lead to member churn.
Healthcare-trained conversation intelligence platforms are built with compliance in mind, using privacy safeguards, redaction, and monitoring to meet HIPAA and CMS requirements. They continuously analyze interactions to detect compliance risks, safety concerns, and documentation gaps across 100% of conversations.
Yes. Conversation intelligence platforms can be tuned to each organization’s lines of business, regulations, workflows, and priorities, whether for Medicare Advantage, Medicaid, or commercial plans. Our AI becomes more precise as it learns your data, processes, and performance goals.
Traditional analytics summarize what’s already known. Conversation intelligence uncovers hidden patterns, emotions, and friction points buried in everyday interactions, turning raw, unfiltered conversations into actionable context.
See Authenticx in action.
Join leading healthcare organizations using conversation intelligence to turn human realities into healthcare impact.
Personalized product demo
Live walkthrough tailored to your use case
Discuss your unique challenges
Custom solutions for your organization
Build a true partnership
Personalized insight analysis and dedicated account support