Artificial Intelligence
The Business of Healthcare is Crushing Care
June 14, 2023 by Amy Brown
Copied link
We have a business of healthcare problem in the United States. This problem is costing us time, energy, trust, money, and, worst of all, our health.
Using artificial intelligence (AI), healthcare-specific machine learning models, and humans who have worked in healthcare, Authenticx analyzed over 100 million healthcare conversations last year. These conversations with patients, caregivers, health insurers, doctors, pharmacy representatives, pharmaceutical manufacturers, and more occur across all verticals of healthcare (e.g., life sciences, hospital systems, health insurers, etc.). Through this analysis, we uncovered a necessity in healthcare that is creating complexities that are crushing care.
This necessity is the business of healthcare. Authenticx Chief Evangelist, Leslie Pagel, and Sally Perkins, Insights Storyteller at Authenticx recently explored this topic in a webinar.
In Looking Back to Leap Forward, Leslie and Sally reviewed what was learned in 2022 to share three things:
- The needs of customers (primarily patients/caregivers)
- How the business of healthcare is going for patients and caregivers
- The actions needed as we move toward 2025
Catch up on the webinar here.
So, what do we mean by the ‘business’ of healthcare?
The business of healthcare includes all steps and stages in the care journey that are associated with paying for care. They include things such as:
- Finding financial assistance
- Understanding out of pocket costs
- Prior authorizations
- Enrolling in patient assistance programs
- Understanding claims and navigating claim denials
- Paying for care
- Selecting an insurance plan
- And many more
The majority of healthcare conversations are about the business of healthcare.
In comparison to the amount of energy that is spent navigating healthcare, there are twice as many customer conversations that are focused on managing the business side of healthcare.
Let that sink in.
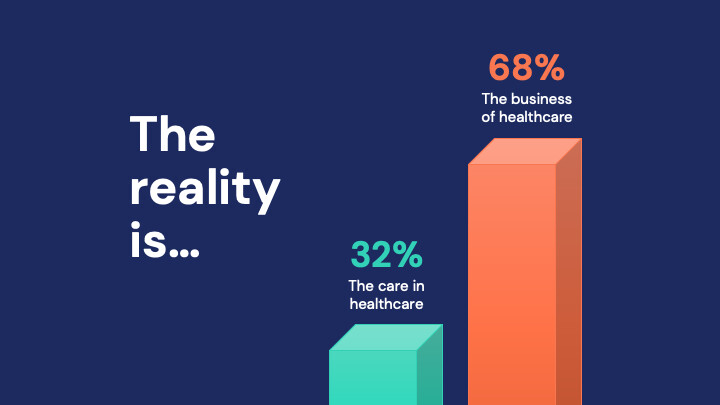
Consumers of healthcare can’t stay narrowly focused on their care because the business of healthcare is looming. And healthcare organizations are spending an enormous amount of money to help patients navigate the business of healthcare.
This is a lose-lose situation.
Coordinating financial coverage is a primary driver of friction.
It’s one thing if the bulk of conversations are about the business of healthcare and those conversations are seamless, but that’s not the case. One of the primary drivers of friction (also known as The Eddy Effect) in the care journey is the coordination of financial coverage.
Patients, caregivers, and doctors get stuck waiting on prior authorizations, navigating the system because of human errors, fumbling through patient assistance programs, trying to understand benefits…the list goes on and on.
What’s the impact of getting stuck? It’s time, effort, and worst of all, access to the care that is needed. Three-quarters of these disruptions and obstacles (we call them Eddies) require additional time – time that they should be spending on their care.
- Nearly half of the Eddies delay or prevent care – keeping them from getting the care they need.
- They are costing us financially – with the average length of an Eddy being three minutes longer than normal interactions.
A Call For Action
The necessity of getting care is encumbered by the business of healthcare. Every decision we make, whether big or small, impacts the patient and their loved ones.
- It’s time we start challenging business norms and start putting the patient at the center of every decision.
- It’s time we start prioritizing the patient’s health alongside business profit.
Where do we get started?
To put the patient at the center of every decision, we must start by listening to fully understand the patient’s needs and responding in a way that communicates, “we hear you.” We must go beyond survey data and start leveraging conversational AI to listen to the lived experiences of healthcare consumers.
As healthcare prioritizes the patient’s perspective and grows more aware of the patient’s voice, initiatives, such as the one highlighted in this example, will begin to reimagine the business of healthcare and crush its complexities rather than to be crushed by them.

Transform CX with Conversational Data
This guide provides the ultimate source of informations about unsolicited feedback and how it can be leveraged to transform your customer experience strategy.
Download the ResourceABOUT THE AUTHOR:
Leslie Pagel is the Chief Evangelist at Authenticx, a conversation analytics company dedicated to improving the way healthcare companies engage with patients. In this role, she creates awareness, across the healthcare industry, of more efficient and effective ways for healthcare organizations to deliver on their customer objectives. With over two decades of working with customer experience (CX) teams, Leslie helps clients actualize the voice of the patient to show how these voices prompt meaningful action.
ABOUT AUTHENTICX:
Authenticx was founded to analyze and activate customer interaction data at scale. Why? We wanted to reveal transformational opportunities in healthcare. We are on a mission to help humans understand humans. With a combined 100+ years of leadership experience in pharma, payer, and healthcare organizations, we know first-hand the challenges and opportunities that our clients face because we’ve been in your shoes.
Want to learn more? Contact us!
Or connect with us on social! LinkedIn | Facebook | Twitter | Instagram | YouTube